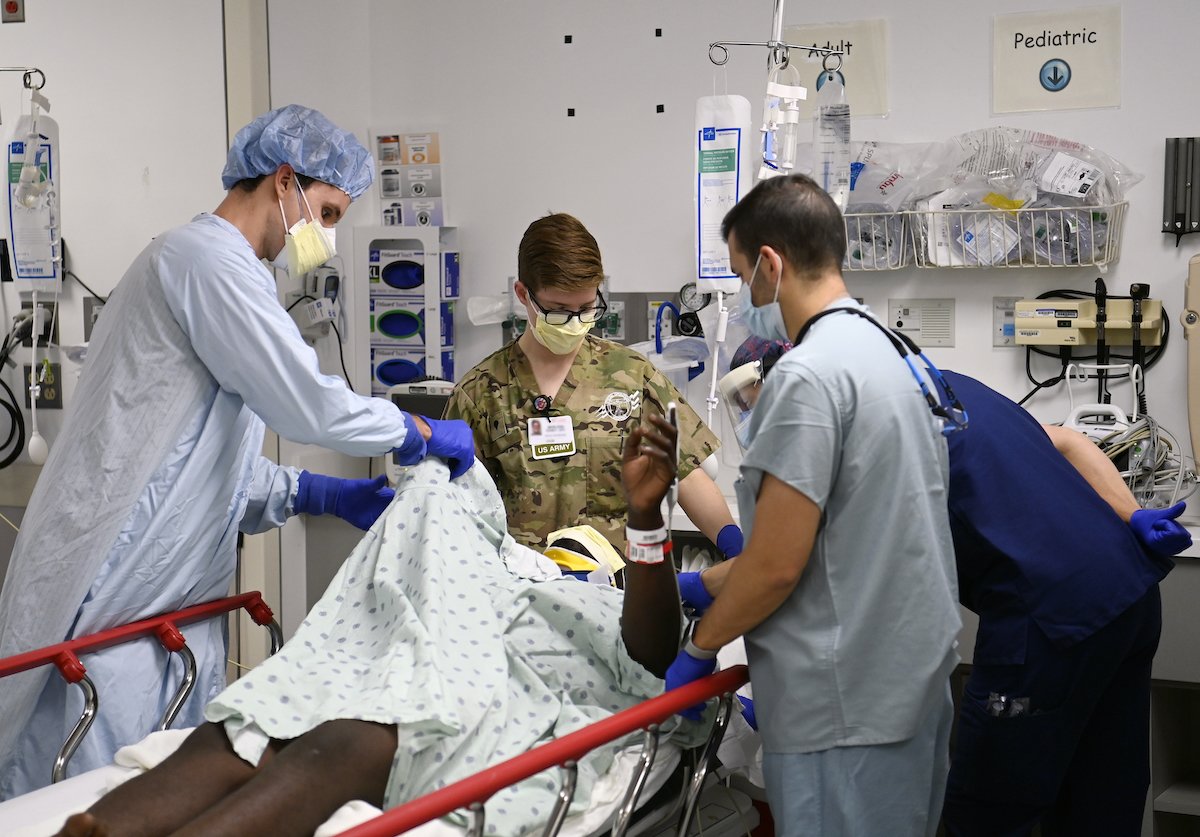
A student from the US Army John F. Kennedy Special Warfare Center and School in the Special Operations Combat Medic Course works alongside emergency medical technicians from Cooper Trauma Center in Camden, New Jersey, June 27, 2021. US Army image by K. Kassens.
The call was two kids inbound with head injuries from a car accident, which is that horrible combination of the worst thing in the world and exactly what Army Specialist M was waiting for.
Specialist M, whom Coffee or Die Magazine is identifying only by an initial due to the nature of their follow-on assignment, was one of three Army medics spread around the emergency room of Cooper University Hospital in Camden, New Jersey, in the final, real-world training phase of the Army’s Special Operations Combat Medic course. The course puts soon-to-be-Special Forces team medics and other SOF troops in Camden for a month to get hands-on training with badly hurt patients, knowing they could each be treating actual combat wounds within months.
Still, the warning of the inbound children instantly affected the ER. The easy banter of the doctors, nurses, and other specialists dropped to zero as tables were cleared and supplies double-checked.
Specialist M moved with purpose and urgency but also a sense of calm. She quickly checked on another patient she had been attending to, adjusting and reapplying bandages and IV lines to ensure they would not need immediate help if the incoming kids needed everyone’s attention.
The truth was, this was far from Specialist M’s first trauma call for kids. She had been a regular Army medic before coming to SOCM and a civilian emergency medical technician before that.

But still.
“It was not my first time seeing kids hurt,” she said. “But it’s still a little bit of a gut check.”
The SOCM students were easy to spot in the Cooper ER, and Specialist M was easy to pick out among them. Unlike the traditionally attired nurses and doctors in green and blue, SOCM students wear camouflage scrubs. And while Specialist M’s fellow students were — like most SOCM students — Special Forces trainees headed for the 18D MOS as SF team medics, she was a battalion support medic for a Special Forces Group and the only woman in a class of 24. She also stood about a head shorter than her classmates as they worked with their patients.
I spent several days with the dozen or so SOCM students as they rotated through two New Jersey ERs and rode ambulances around Camden, serving a county of about half a million adjacent to Philadelphia. Camden is a hard city with a high poverty rate and a long history of gun violence and other ills. As a result, Cooper is one of the busiest ERs in the country.
Specialist M’s trip to SOCM started about 200 feet in the air.
On what she figures might have been her seventh jump — “I was still a baby paratrooper,” she said — she watched as one jumper in her stick slipped below another jumper, “stealing” that jumper’s air and all but collapsing their parachute. As she floated downward, Specialist M watched the higher jumper plummet and hit the ground hard, obviously injured.
Almost immediately, she spotted a single figure, already free of his harness, running toward the hurt soldier.
“He was already tearing across the ground,” she said. “It was awesome.”
The sprinting soldier was, like Specialist M, a medic — a “68-Whiskey,” in Army MOS parlance — but he had just graduated from SOCM. Even under canopy, she could see his sense of purpose and skills. The jumper’s injury was gruesome — a compound femur fracture and, Specialist M remembered, “his foot was kind of sideways” — but the medic never flinched.
“The way he did his primary survey and processed that trauma, the calmness and collectedness he worked with,” she said. “I was very interested in the skill set he had, and when I asked about the training he’d been through, I thought, ‘Cool, okay, I want to do that.’”
Specialist M spent the next year trying to get a slot to SOCM as a battalion support medic. While SOCM has long been a training ground for team-level special operators, including Green Berets, Rangers, Navy SEALs, Marine Recon, MARSOC medics, and in the past, Air Force Pararescue. But the course has expanded over the years to include other special ops-centered roles. The 24 students in Specialist M’s class included flight medics with the 160th Special Operations Aviation Regiment, battalion support medics like Specialist M, and Civil Affairs medics. Specialist M’s first shot at SOCM ended when her home unit in the Nebraska Guard, where she’d witnessed the parachuting accident, folded. However, that led her to transfer to a Special Forces Group which regularly sends unit medics to the course (a process outside the path for the unit’s Green Berets, who qualify through the traditional Special Forces operator pipeline).
But there were far more medics who wanted in than there were slots available.

To win a spot, Specialist M entered a five-day selection with 12 hopefuls. The trial included physical fitness tests, ruck marches, and medical evaluations. In one of the final medical drills, she noted to her examiner that the “patient” needed a blood transfusion. A bio-med major in college before joining the Guard, Specialist M had recently read up on the use of whole blood by military medics in the field, a major change in protocol from blood plasma and other products of the past decade.
“I read a lot,” she said. “I stay up on my protocols.”
As she assessed, treated, and packaged her patient for transport, she kept up a discussion with her evaluator, an SF team medic, on the benefits of whole blood and the methods she would use, if allowed.
“I told him that whole blood is actually indicated here, and here’s why,” she said.
In the end, the unit sent two soldiers to SOCM, including Specialist M.
Getting in, though, was the easy part. While the idea of “Special Forces training” elicits images of low-crawling through mud pits and punishing ruck marches, SOCM has very little of that. However, its attrition rate is still higher than that of Ranger School.
The first cut is academics, with a firehose course of basic anatomy, physiology, and clinical knowledge, for which Specialist M found herself well suited. Then comes the real grinder: the hands-on trauma care that culminates in a series of simulated combat scenarios in which medics have just minutes to assess and treat a series of gruesome “injuries” on patients and evacuate — or move “off the X.”
Miss an injury, fail to open an airway, blow an IV, incorrectly wrap a bandage, misreport a vital sign, or make one of a dozen other potential mistakes, and you are a no-go.
“As Trauma progressed, I was feeling myself getting better,” Specialist M said. “They grade the practice lanes, and seeing my feedback change there was a really big confidence builder — like, ‘Okay, I do know what I’m doing. I can be a little bit calmer in these scenarios.’”
The final phase is real-world rotations in Camden or one of several other cities. Students pull 12-hour shifts for a month with few days off, riding with ambulance crews and working side by side with ER staff.
On Specialist M’s first hospital shift, a patient arrived who had been hit by a car. Their lungs were collapsing from internal injuries.
“The trauma doc is looking at you like, ‘All right, chest tube, go,’” Specialist M said. She had to cut a hole in the man’s side and spread apart the muscle and tissue around his ribs, then, using a pair of clamps, shove a rubber tube inside his rib cage to release the building pressure.
However, unlike in the calm, by-the-book world of SOCM training, the ambulance medics were still pounding away on the man’s chest, doing CPR.
“I am holding a scalpel, and I’ve never cut on something that, you know, was being compressed on,” she said. “The doc is like, ‘Just yell at them!’”
So she did: “Hold CPR!” she yelled. The compressions stopped. She cut, spread, and jabbed the tube in. She listened for the hiss of air escaping from the man’s chest. CPR started again.
This was real-world training.
“It was the coolest thing ever,” Specialist M said.
Working in the hospitals, she scrubbed in on three neurosurgeries and, under a surgeon’s watch, was allowed to drill into one patient’s skull. But she also found challenges in more mundane calls.
“It’s definitely been humbling to try to get IVs on dehydrated old ladies,” she said.
As the only woman in the class, she said, she’s met only one person who objected to her presence: “My dad is not the biggest fan of my choice. It’s a very traditional family, and it’s not a very ladylike thing to do. But my mom’s a fan, though she worries a lot. My brother thinks I’m completely crazy.”
Back at Cooper, another call came through: The kids weren’t coming. They diverted to a children’s hospital in Philadelphia, one of the few places in the region more equipped than Cooper to deal with the particulars of pediatric care.
Specialist M and the other two SOCM students relaxed, but only a little. There would be more. And they’d be ready.
This article first appeared in the Fall 2021 edition of Coffee or Die’s print magazine as “Preparing for Trauma.”
Read Next:
Matt White is a former senior editor for Coffee or Die Magazine. He was a pararescueman in the Air Force and the Alaska Air National Guard for eight years and has more than a decade of experience in daily and magazine journalism.