‘We Need To Fix This’: Competing Veteran Health Bills Seek To Address Toxic Exposures

US Marine with the Warfighter Exchange Service Team (WES Team), Combat Logistics Regiment 2, walks away after disposing of trash at the burn pit in Forward Operating Base (FOB) Zeebrudge, Helmand province, Afghanistan, March 6, 2013. The WES Team travels to Patrol Bases and FOBs from Camp Leatherneck to provide PX supplies, cash and postal services to fellow deployed servicemembers that are normally not accessible. US Marine Corps photo by Sgt. Anthony L. Ortiz/Released, courtesy of DVIDS.
In the summer of 2018, Oscar Olvera was sitting at a bar, complaining to his friends that he had been “feeling weird” with aches and pains. That fall, he developed migraines and fatigue so severe he missed a month’s worth of school and ultimately had to drop out. He went to a VA doctor who did some blood work but couldn’t find anything wrong. The next spring, a vein in Olvera’s neck started popping out. Several visits later a doctor ordered a chest X-ray, revealing numerous tumors.
“I was 28 years old, and I had lung cancer,” Olvera said. “That doesn’t happen. That’s just not a thing.”
According to the American Cancer Society, the average age at which a person is diagnosed with lung cancer is 70.
Lawmakers in both chambers of Congress have introduced three different bills to care for veterans poisoned by toxic environments overseas. They disagree on the best approach, resulting in the competing bills and concerns from some veterans.

Currently, veterans seeking treatment and VA disability compensation for exposure to burn pits or other toxic materials or environments must show that their health problems are linked to contact with certain environmental hazards while serving in the military. The VA lists several specific locations and environmental hazards as eligible for coverage, but it can be extremely difficult for some veterans to prove they had contact with toxic materials, including “particulate matter or large burn pits.”
The Presumptive Benefits for War Fighters Exposed to Burn Pits and Other Toxins Act is a bipartisan bill championed by US Senators Marco Rubio (R-FL) and Kirsten Gillibrand (D-NY). The bill would remove most of the burden of proof from veterans, instead providing presumptive VA benefits to anyone who can prove they earned a campaign medal connected to the War on Terror and that they suffer from one of a long list of illnesses.
Qualifying illnesses include numerous types of cancer, chronic bronchitis, constrictive bronchiolitis, emphysema, and more.
A similar bill was introduced last year but failed to gain traction. Chelsey Poisson is a former Army medic and the executive director of the HunterSeven Foundation, a nonprofit dedicated to helping veterans impacted by toxic exposures. Poisson told Coffee or Die Magazine she believes the Rubio-Gillibrand bill is destined for the same fate as last year’s bill because its massive expansion of the eligibility pool makes it extremely expensive.
According to a 2015 VA report, as many as 3.5 million veterans may have been exposed to burn pits in Afghanistan, Djibouti, and the Southwest Asia theater of operations.
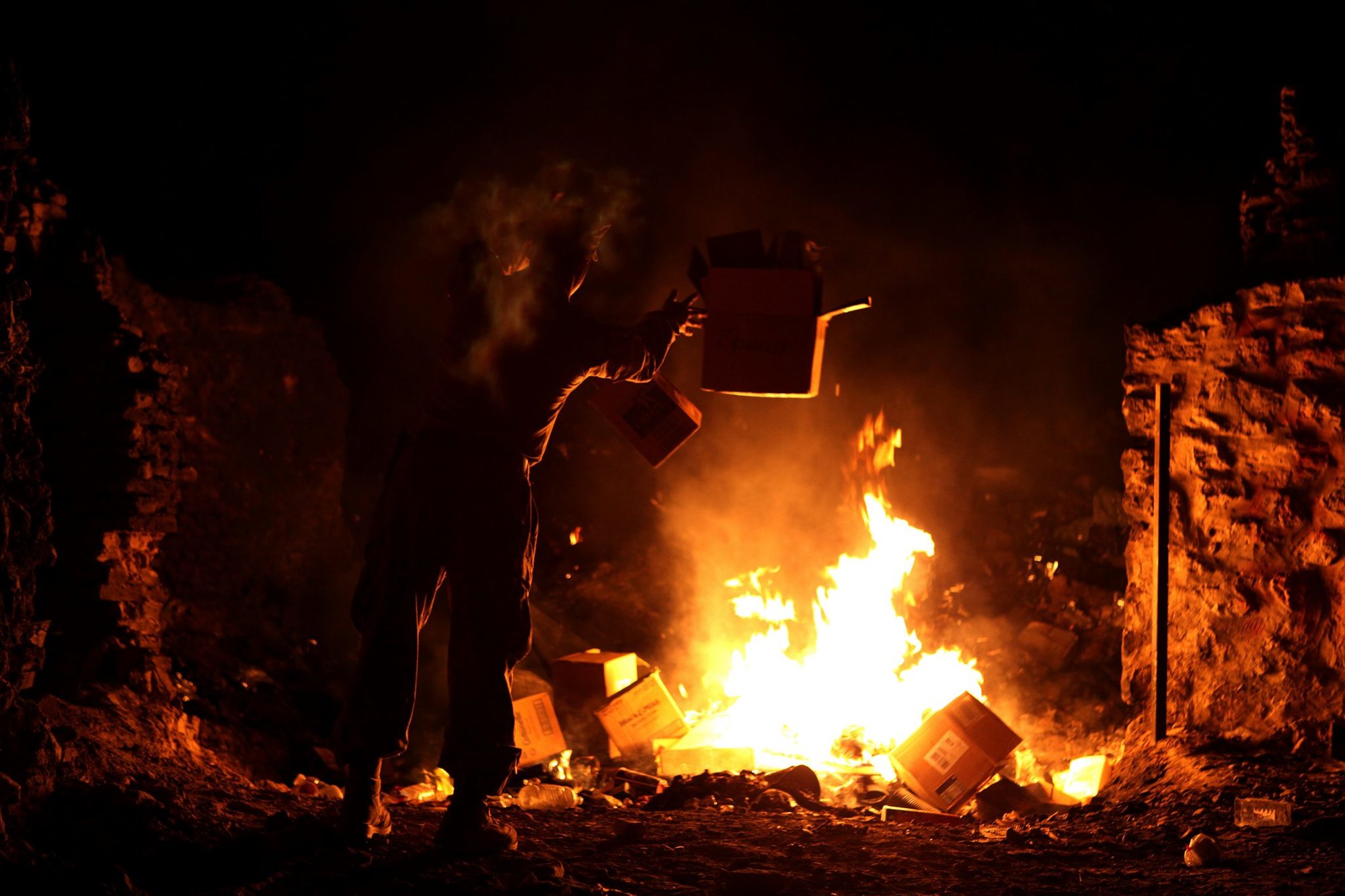
For decades, the military has used burn pits to dispose of trash on combat outposts and bases overseas, burning everything from plastic to food scraps, tires, human waste, and more.
“Smoke and other emissions from these pits contained an unknown mixture of substances that may have short and long-term health effects,” reads the VA report on burn pits. According to the VA, 96% of survey participants said they were near a burn pit on at least one of their deployments.
However, most didn’t spend time thinking about the dangers of breathing toxic fumes.
“We had the immediate risks of, you know, IEDs, getting shot at and stuff,” Olvera said. “You didn’t really care about the smoke in the air or what you’d been exposed to because you were more concerned about whether or not you were gonna get your legs blown off.”

Many veterans and active-duty military members struggle to get an accurate diagnosis when they seek help.
Poisson, who is also an ER nurse, said age was part of the problem. If she sees a 30-year-old and a 60-year-old with the same exact symptoms, without knowing whether the younger patient has been exposed to toxic environments, the older patient will likely get more attention. The consequences are deadly.
Army Staff Sgt. Ron Shurer II, who was awarded the Medal of Honor in 2008 and went on to serve in the Secret Service, died at 41 from lung cancer. Doctors initially attributed his shortness of breath and debilitating hip pain to his active lifestyle, not finding the tumors covering his lungs and spine for nearly a year.
Joint Terminal Attack Controller Luke Page died at 31 from cancer that was misdiagnosed and mistreated for more than a year.
Master Sgt. Geoffrey Dardia, now 44, started suffering from fatigue, migraines, balance problems, double vision, and other symptoms in 2007.
“It was like getting hit in the head with a brick,” Dardia said. He went to the doctor. The doctor said he was fine. Dardia continued teaching high-intensity courses to fellow Green Berets, spending massive amounts of time in shoot houses where he was consistently inhaling lead, mercury, and other heavy metals, he said.

About five years after noticing symptoms, he started looking into what could be causing his problems and learned about toxic exposures. In 2012, he reached out to a doctor at Walter Reed Medical Center who agreed to evaluate him.
The results showed that his bone lead levels were about twice the normal amount, Dardia said. His mercury and arsenic levels were even worse.
“[The doctor] was like, ‘What the hell happened to you?’” Dardia recalled. The doctor had just started working with special operations forces and described the group to Dardia as “packed full of toxins.”
“But, you know, none of us expected to live to face the long-term effects,” he said. When he’d seen that doctor, five years after returning from deployment, Dardia realized that, if he wanted to continue living, he’d have to change. “That was my come-to-Jesus moment.”

After going through a treatment called chelation, which helps the body excrete toxins, Dardia is doing much better, despite lingering cardiovascular and nervous system issues.
Dardia went on to team up with the Task Force Dagger Special Operations Foundation, which assists sick or injured US Special Operations Command members and their families. His focus is on educating military members and leadership in an effort to prevent illness in the first place.
“You can’t protect yourself against something if you don’t know what the threat is,” he said. “People are dying right now because we’re failing to educate them on these things.”
Two bills recently announced by legislators focus more on education and prevention.
Congresswoman and Navy veteran Elaine Luria (D-VA) announced the COVENANT Act earlier this month. Like the Rubio-Gillibrand bill, it would presume that veterans who served in specific regions were exposed to burn pit hazards. Unlike the other bill, though, it includes a clause reading, “unless there is affirmative evidence to establish that the covered veteran was not exposed to any such airborne hazard during such service.” The COVENANT Act includes a (slightly different) list of 15 qualifying diseases, including several types of cancers, but it would allow veterans to submit claims for additional illnesses, in which case they would be provided a medical examination to determine whether the illness could have been caused by a long list of airborne hazards.

What sets the COVENANT Act apart from the Rubio-Gillibrand bill is that it would also necessitate relevant training for VA medical providers on airborne-hazard-related illnesses and unexplained, chronic, multi-symptom illnesses.
Senator Tom Tillis (R-NC) has also reintroduced his 2020 TEAM Act. Like the other bills, it would expand benefits for veterans exposed to toxic substances. It would further direct the government to study exposure to toxic substances, improve outreach to exposed veterans, and better train healthcare personnel to recognize potential exposure.
The Congressional Budget Office has not yet studied the financial impacts of any of the legislation.
Marine Corps veteran Zachary Bell, who gained internet fame as Veteran With A Sign, told Coffee or Die Magazine he’s glad something is being done but feels the issue could have been addressed sooner. Bell, who deployed twice to Afghanistan, said burn pits were everywhere during his deployments, sometimes within 100 feet of sleeping areas. After leaving active duty, Bell noticed rashes and other skin problems. It turned out to be dermographism, also known as “skin writing,” a condition where the skin produces an exaggerated healing tendency when stroked, he said.

“Basically my skin is always agitated and it can get so bad that I go into anaphylactic shock,” Bell wrote in an email. “When my kids were little they couldn’t cuddle me because my skin would get so bad.”
Bell doesn’t know yet which bill is the best option, and none include his condition as a qualifying illness. But he’s adamant about one thing: “We need to fix this.”
Olvera, who is now in remission and plans to return to school and finish his physics degree once the side effects of chemo wear off, said no matter what happens in Congress, prompt treatment was key for helping veterans like him survive.
“There were a lot of stories out there of soldiers going to sick call with symptoms and then their symptoms being brushed aside and ignored until it’s too late,” he said. “That’s what the VA and the military really need to focus on.”
Read Next: Veteran with Lung Cancer From Burn Pits Seeks Changes to VA, DOD Benefits

Hannah Ray Lambert is a former staff writer for Coffee or Die who previously covered everything from murder trials to high school trap shooting teams. She spent several months getting tear gassed during the 2020-2021 civil unrest in Portland, Oregon. When she’s not working, Hannah enjoys hiking, reading, and talking about authors and books on her podcast Between Lewis and Lovecraft.
BRCC and Bad Moon Print Press team up for an exclusive, limited-edition T-shirt design!
BRCC partners with Team Room Design for an exclusive T-shirt release!
Thirty Seconds Out has partnered with BRCC for an exclusive shirt design invoking the God of Winter.
Lucas O'Hara of Grizzly Forge has teamed up with BRCC for a badass, exclusive Shirt Club T-shirt design featuring his most popular knife and tiomahawk.
Coffee or Die sits down with one of the graphic designers behind Black Rifle Coffee's signature look and vibe.
Biden will award the Medal of Honor to a Vietnam War Army helicopter pilot who risked his life to save a reconnaissance team from almost certain death.
Ever wonder how much Jack Mandaville would f*ck sh*t up if he went back in time? The American Revolution didn't even see him coming.
A nearly 200-year-old West Point time capsule that at first appeared to yield little more than dust contains hidden treasure, the US Military Academy said.












